I got my first COVID-19 vaccine on December 18th, 2020
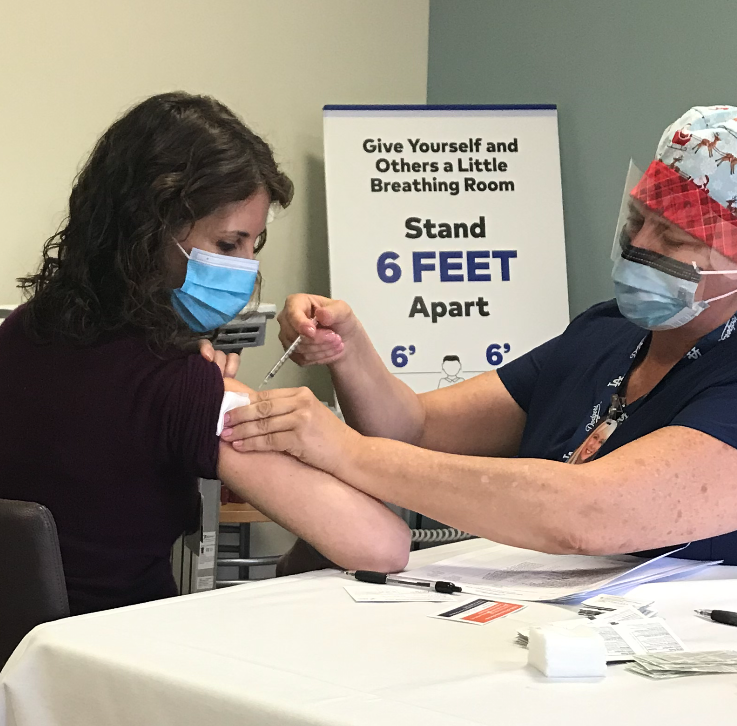
I was fortunate to be amongst the first people to get the COVID-19 vaccine as a healthcare provider. I got my first dose of the Pfizer vaccine on December 18th, 2020, and will get my second dose on January 7th, 2021.
Like many of you, I had a lot of questions and hesitations before the vaccine was officially available, so I did A LOT of research in the past several weeks to find the answers. I am writing this newsletter to share my findings with you.
Before I start, let me point out (in case you did not notice!) that the woman administering the vaccine in this picture is not wearing gloves. And although I personally wear gloves for all procedures, the Occupational Safety and Health Administration (OSHA) regulations do not require gloves to be worn when administering vaccinations, unless persons administering vaccinations have open lesions on their hands or are likely to come into contact with a patient’s body fluid.
What is the COVID vaccine
Most vaccines work by injecting the body with a weakened or inactive virus, which then activates the immune system to build protective antibodies against the virus.
The COVID vaccine utilizes a unique technology that does not require either dead or inactive virus to enter our bodies. Instead, a synthetic (ie made in the laboratory) protein called mRNA is injected into the body.
What is mRNA
Here is a brief overview of the science. I will try to keep it simple!
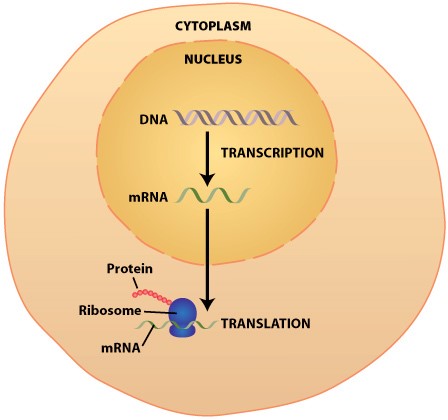
Picture from https://sites.duke.edu/apep/module-2-the-abcs-of-intoxication/biology-and-chemistry-connections/dna-transcription-translation-synthesis-of-proteins/
Our genetic material is embedded in our DNA. The DNA resides in each cell of our body inside of the cell’s nucleus, where it is protected from damage. When specific proteins are needed by the cell, DNA makes messenger RNAs, or mRNAs. Each mRNA has the recipe to make a specific protein. mRNA leaves the nucleus and enters the cytoplasm of the cell. There, with the help of various proteins that exist in the cytoplasm, the cell makes the protein that is coded by the mRNA.
Since about 2005, the scientists have worked on a technique using mRNA as a vaccine. This brilliant technique would eliminate the need to inject the body with the virus at all; instead, by using a replica of the virus’ mRNA, our body would be tricked into making a virus protein in our own body. In January of 2020, at the very beginning of the pandemic, the scientists determined the genetic code of COVID-19, hence the recipe for all the proteins it can make. The COVID virus has a protein on its surface called the spike protein. This is the protein that our immune system would recognize as foreign and would make antibodies against, when the virus is in our body.
The COVID-19 vaccine is a synthetic (man-made) copy of the mRNA that codes for the spike protein. Since mRNA is very fragile, it is put in a lipid (fat) capsule to make it more stable and easier to enter the cell. With the lipid capsule, the mRNA is able to enter the cell, but it is not able to enter the nucleus, where our DNA safely resides.
Our cells see the mRNA and, like they would with mRNA produced by our own DNA, use the ingredients in their cytoplasm to make the spike protein that the mRNA has coded. However, once the spike proteins are made, our body quickly realizes that this protein was not coded by our DNA, and alarms the immune system to fight this foreign protein. Our immune system creates antibodies to the spike protein and destroys it. Once the antibodies are made, they stay around waiting to destroy any of the same spike proteins that come their way. This is how we get immunity against the virus. So if the COVID virus enters the body of a vaccinated person, the antibodies very quickly attach to the spike protein on the virus and destroy it before it has a chance to do any damage to the body.
Questions you may have about this vaccine:
When can I get the vaccine?
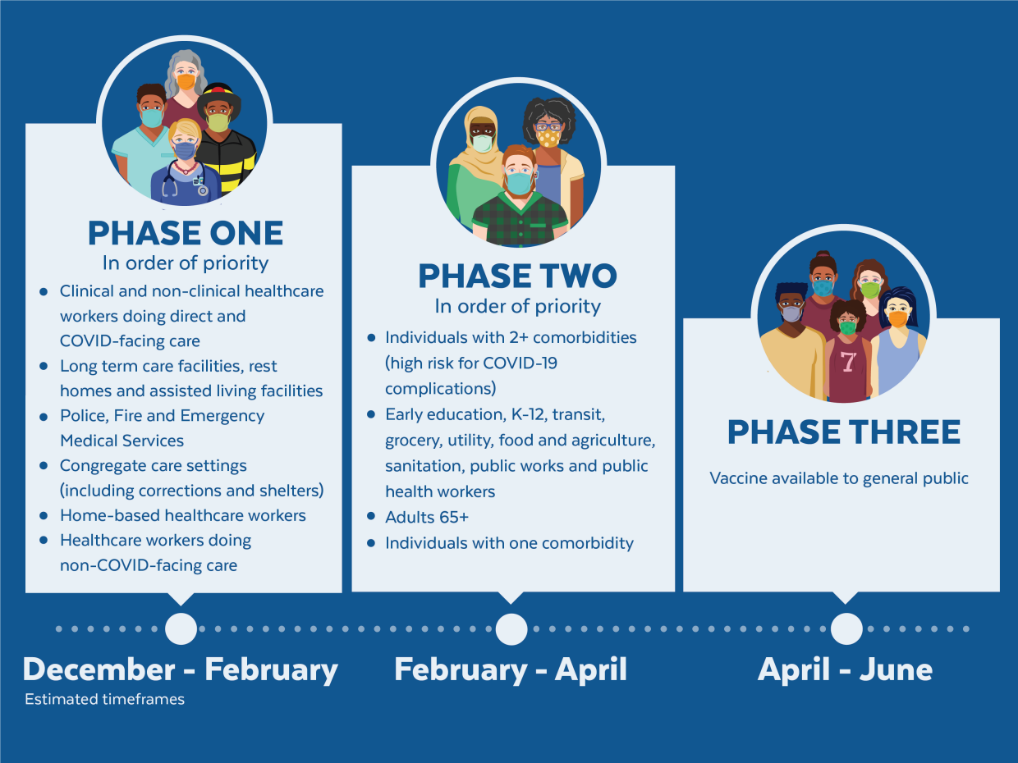
Most healthcare workers and people in nursing homes started getting their vaccines in the middle of December. California is still developing its timeline for the vaccine, but most others who already have a timeline look something like this:
From: Massachusetts vaccine advisory; https://www.mass.gov/info-details/when-can-i-get-the-covid-19-vaccine
Who are people with comorbidities that put them at higher risk for COVID-19?
People with diabetes, lung disease, and those who are immune suppressed, among others. In the rheumatology world, those of you taking immunosuppressive medications (mostly biologics, high dose prednisone greater than 10mg/day).
What are the side effects of the vaccine?
The CDC lists the following as the potential side effects:
Pain and swelling at the site of the injection- usually lasts 1-2 days
Fatigue, chills, headaches, and less commonly fever- also lasts 1-2 days
I had a very sore arm for about 24 hours. Most people I have talked to have reported the same.
Most people can use Tylenol or Advil to treat these symptoms. If your symptoms are more severe, you will be calling your physician.
Note that side effects are more likely to occur with the second dose of both vaccines. It seems that they may also be more common if you have already had COVID-19 in the past and still have some circulating antibodies. Still, it is recommended that you get the vaccine if it has been longer than 90 days since you had COVID-19, since it is thought that natural antibodies don’t last longer than that therefore you are still susceptible to catch the disease.
Which vaccine should I get?
There are currently two vaccines available to us:
Pfizer vaccine: 2 injections, second injection 21 days after the first, 95% immunity reached one week after the second shot.
Moderna vaccine: 2 injections, second injection 28 days after the first, 94.5% immunity reached two weeks after the second shot.
The Pfizer vaccine needs to be shipped and stored at minus 94 degrees Fahrenheit, while the Moderna vaccine can travel and be stored at minus 4 degrees Fahrenheit.
The Pfizer vaccine was studied on 44,000 subjects; and the Moderna one on 30,000 subjects.
Conclusion: both vaccines are about the same, so it really doesn’t matter which one you get. Which vaccine you get will likely depend on which one will be available to you. I suspect other than large hospitals, most places do not have a minus 94 degrees freezer so what will be available at the pharmacy or the doctor’s office will most likely be the Moderna one.
Can I still get COVID even after I get the vaccine?
95% efficacy is reached after 2 doses with both vaccines. This takes 4 weeks with the Pfizer vaccine (three weeks between the two doses plus one week after the 2nd dose to reach maximum efficacy), and 6 weeks with the Moderna vaccine (four weeks between the two doses plus two weeks after the 2nd dose). If you are exposed to COVID after each time period, your chance of getting the virus is about 5%. If you are exposed within this period your chance is higher.
If I already got COVID, can I assume I am already immune and don’t need the vaccine?
Unfortunately not. The data has shown that the antibodies formed after getting COVID-19 are short lasting; and generally disappear in about 90 days. Although it is not yet definitive how long the antibodies from the vaccine last, the currently available data show that they last longer than those from natural immunity.
Can I stop wearing a mask once I am vaccinated?
The short answer is not yet, and we don’t know yet for sure.
At this time it is not clear if the vaccine will prevent you from getting the virus altogether, or only prevents you from having symptoms. If you are able to still get the virus without being symptomatic, you can still pass it on to others who are not vaccinated. So it seems we may have to still be diligent with wearing our masks until the majority of people are vaccinated.
Also, if you have a 95% immunity after vaccination, but many people around you have the virus, you still have a 5% chance of getting the virus. But if everyone around you also has a 95% immunity, then the cumulative risk becomes very, very small to each of you.
Can I have an allergic reaction to the vaccine?
Allergies to vaccines happen, and the COVID-19 vaccine has been no exception.
This is what the CDC recommends:
“If you have ever had a severe allergic reaction to any ingredient in a COVID-19 vaccine, CDC recommends that you should not get that specific vaccine. If you have had a severe allergic reaction to other vaccines or injectable therapies, you should ask your doctor if you should get a COVID-19 vaccine.
CDC recommends that people with a history of severe allergic reactions not related to vaccines or injectable medications—such as allergies to food, pet, venom, environmental, or latex—may still get vaccinated. People with a history of allergies to oral medications or a family history of severe allergic reactions, or who might have a milder allergy to vaccines (no anaphylaxis)—may also still get vaccinated.
If you have a severe allergic reaction after getting the first shot, you should not get the second shot. Your doctor may refer you to a specialist in allergies and immunology to provide more care or advice.”
Was the COVID-19 vaccine rushed?
Remember that the mRNA vaccine technology has been studied since 2005. The genetic code of the COVID-19 virus was available in January 2020. The vaccine itself was made within a couple of months (recall all the news about it back in April) of that, but it still took several months for it to go through the usual rigorous testing required to get it approved by the FDA.
So was the vaccine produced really fast? You bet. But rushed? Hardly.
Usually vaccine development requires millions of dollars of funding. After each step of the research (in vitro studies, animal studies, phase I, II, and III studies), the researchers have to go back to the funding source, provide results, and apply for more funding for the next phase. This often takes a long time (of waiting around) as funding is limited. However, in the case of this worldwide pandemic, the vaccine got priority over all other vaccines being developed. Funds were made readily available, which enabled the scientists to focus on completing each phase efficiently rather than waiting around for funds.
“What about studies about long term side effects?”, you may ask.
It is true that it takes about 2 years after development of any drug to study long term side effects. However, the data from other vaccines show that usually 97% of the side effects happen within the first 6 weeks of vaccination. The phase 3 vaccine trials started back in July, and all recipients completed their two doses by November (some sooner). So there is definitely more than 6 weeks of data is available post vaccination. And by the time many of you get the chance to get the vaccine, even more time and data will have accumulated.
But 2 years? I would argue that we don’t have that kind of time to wait. My colleagues that work in the hospital share horror stories about how the ICUs have filled up and there are no hospital beds, how they and the hospital nurses are tired and overworked, and how many patients are dying in front of their eyes every day. I may not believe what I hear in the media, but I do believe these firsthand stories from frontline physicians.
And if you, like me, have been on Facebook lately, you may be seeing posts and pictures of healthcare workers excitedly getting their vaccines. This is because we are realizing that all our efforts of social distancing, mask wearing, and closing down businesses have not been effective in controlling this virus. We need to do something different. And most of us believe this is how we can end this pandemic.
Will the vaccine will change your DNA?
No, this is not possible. This is an mRNA vaccine and does not contain any DNA, and cannot insert itself into or change your DNA. Furthermore your DNA is well protected inside the nucleus. The synthetic mRNA in the vaccine is incapable of crossing the nucleus barrier to get in.
Can this vaccine cause an autoimmune disease?
There have been no evidence of an autoimmune response in either trial for the vaccines.
Will the vaccine cause Bell’s palsy?
A number of cases of Bell’s palsy were reported in the COVID-19 vaccine trials. Specifically 7 people in the two studies (ie. 7 people in ~74,000 people), got Bell’s palsy. This was no higher than the rate of this condition in the general population, therefore it is thought not to be connected to the vaccine.
Can I catch the virus from the vaccine?
No. There is no live or dead virus in the Pfizer or Moderna vaccine. mRNA is just a protein (recipe) for our own cells to make the spike protein. The mRNA has a half life of 2 weeks. This means that half of the protein is out of our system in 2 weeks. The rest is out by 2 months, so theoretically there should not be any long term side effects from this vaccine.
COVID-19 has a survival rate of 99%. Why wouldn’t I just take my chances?
There are three major reasons I can think of:
If everyone else is vaccinated I don’t need one
Think about the diseases that have been eradicated for decades with vaccines- Polio, Smallpox and Measles. We almost forgot about these diseases, didn’t we? Then a small group of people opted not to vaccinate their kids and Measles started popping up again. Vaccines work when the majority of people use it. It is estimated that for this vaccine to be effective, about 70% of people need to get vaccinated. However to truly eradicate COVID-19, nearly 100% of the population would need to get vaccinated.
Are there microchips in the vaccine?
To people who are afraid that the government is planning to inject them with a microchip in the vaccine to track their movements I say this:
Can the vaccine make women sterile?
There have been some social media hype claiming that “the vaccine contains synctin-1, which is vital for the formation of human placenta, so could lead to infertility”. The argument is that the spike protein is similar to a protein on the placenta, so if we make antibodies to the spike protein, the antibodies can also attack the protein on the placenta therefore making women sterile.
Fortunately, there has been no evidence of this. In the Pfizer trial, despite instructions to use birth control, 23 women did get pregnant. About half of these women were in the vaccinated arm, and the other half got placebo. Also, when looking at those women who already got COVID, we don’t see pregnancy loss or infertility, even though they would have gotten natural antibodies from getting the disease.
Is the vaccine safe in pregnancy and breastfeeding?
Although several people who got the Pfizer vaccine did get pregnant, neither the Pfizer or Moderna vaccine has been specifically studied in pregnancy or breastfeeding. Moderna has completed animal studies looking for evidence that the vaccine might harm the pregnancy or the developing fetus, and has not seen such signals. Pfizer has only interim data from its animal studies, and also reports no concerning data so far. At this time, the official recommendation is that each pregnant of breastfeeding woman discuss and weigh the benefits and potential risks with their physician in order to decide if the vaccine may be beneficial in their case.
Will the vaccine be given to children?
Both vaccines were studied in adults 16 years and older, and currently are not recommended in the younger age group, until further data becomes available. Trials are currently ongoing for children 12 years and older and we expect the data to be available in a few months.
How long will I be immune?
We don’t know yet for sure how long immunity from the vaccine will last. As more time passes from the start of the vaccine trials, this will be more clear.
What we also don’t know is while the vaccine prevents us from getting symptomatic COVID-19 infection, if it also prevents us from shedding the virus and passing it to others while being asymptomatic ourselves.
The answer to some of these questions will be more clear over the next few months.
Further reading: